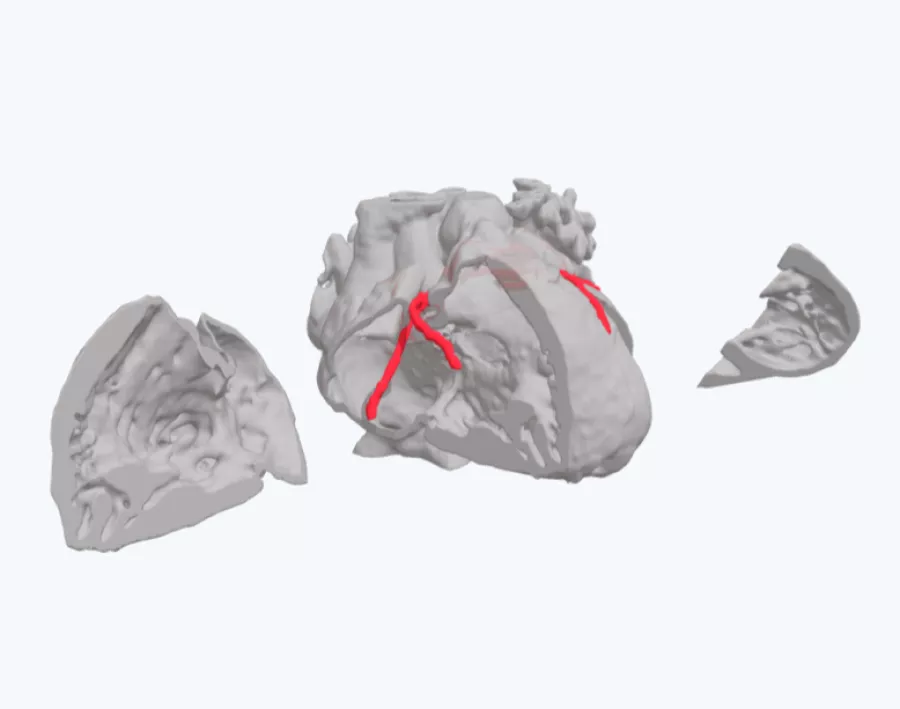
3D Printed Model Helps Clinical Team Plan Surgery for Infant with Multiple Heart Defects
CHD affects approximately 1 in 100 live births, making it one of the most common congenital anomalies. The severity of CHD can vary widely, ranging from minor defects that require no medical intervention to complex conditions demanding immediate surgical intervention.
The most common type of heart defect is a ventricular septal defect (VSD). Many VSDs are small and close on their own, however in some cases there are further complications, such as in this case, where surgical intervention is often required.
Case
A male infant presented with a combination of heart defects encompassing a sizable and intricate inlet VSD, an aortic arch hypoplasia stemming from an underdeveloped aorta, a coarctation caused by a narrowing of the aorta, and a minor obstruction in the left ventricular outflow tract (LVOT) at the aortic annulus.
The intricate amalgamation of these diverse heart defects extended beyond cardiovascular implications to impact his pulmonary function. The left lung had collapsed, and the right lung had also been compromised, leading to respiratory challenges.
Solution
The medical team needed to prepare themselves for an intricate surgical procedure - a biventricular repair involving VSD closure, as well as the replacement of a compromised aortic valve with a pulmonary valve. To ensure the optimal surgical strategy, the surgeons requested a 3D printed replica of the boy's heart, enabling them to validate their approach before proceeding.
Benefits of the 3D Model
The model played a vital role in facilitating the team's assessment of different repair options, providing a clear basis for choosing one approach over another. This unified view of the patient's heart proved invaluable to every team member, offering comprehensive insight before entering the operating room.
Yet, the advantages of the model extended further. Recognizing the understandable concerns of the child's family regarding the upcoming surgery, the doctors were empowered to provide complete information and education about his condition. This not only highlighted the critical nature of their actions but also reassured the family that the chosen path was not only the safest but also the most optimal for the child's recovery.
Disclaimer: Details of Axial3D's regulatory clearance for diagnostic use cases are outlined here . For all other uses of Axial3D solutions, they should be used for demonstration and education purposes only.
Talk to an expert about an upcoming case to see the benefits a 3D printed model can provide.
Contact us.