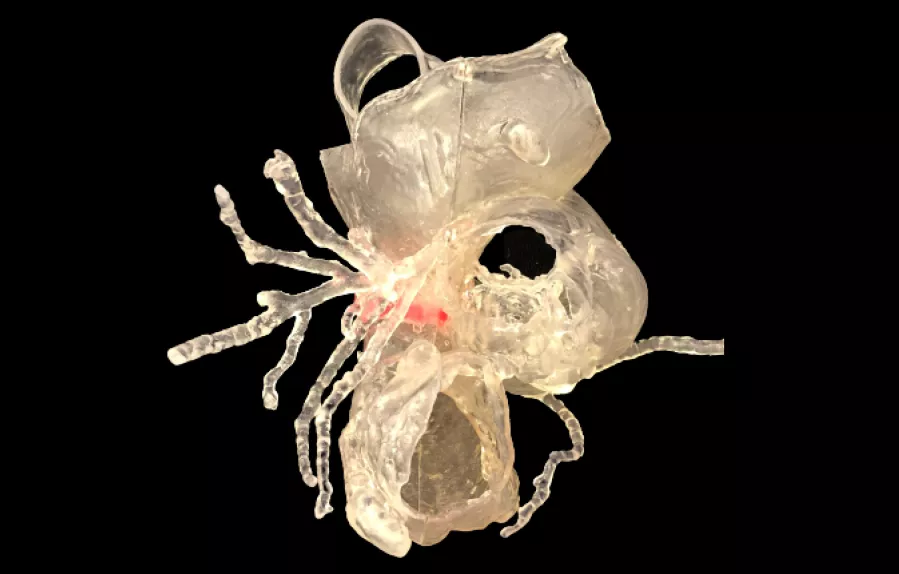
3D cardiac model supports Hancock valve replacement
Case
A 20-year-old female presented with pulmonary atresia with VSD. A previous Hancock conduit required revision and stenting. It was difficult to assess the distance of the replacement site with coronary branches, so the surgeon requested a 3D printed model to augment the 2D scans. The CT scans were used to create a 1:1 scale model in clear resin with the Hancock valve contrasted in red.
Given the history of multiple cardiac surgeries, further sternotomy and cardiac surgery would be of significant risk - therefore a transcatheter solution was preferable. The location of the Hancock valve and its relationship to coronary anatomy was key for this procedure.
"The key advantage was being able to accurately model the coronary arteries and their relationship to the pulmonary outflow tract (i.e. where the valve would be placed); as with inflating balloons in the pulmonary outflow there is a risk of coronary compression and therefore significant complications. Having the 3D model allows for a better safety margin, we are more confident to proceed with the case knowing the exact relationship between these critically important blood vessels."
- Mr Christopher Lockhart MB BAO BCh (Hons) MD, Royal Victoria Hospital, Belfast
Outcome
The consultant was provided with a 1:1 scale 3D printed model of the aorta, pulmonary artery and left and right coronary arteries. The model was produced as a clear print and the Hancock valve in the pulmonary artery was contrasted in red to highlight the relationship of the Hancock valve to the coronary anatomy. The model was then used by the clinician to assess clearance space between the new stent site and coronary vessels.
Having access to the 3D anatomical model meant that the patient was fully informed and consented prior to surgery. The surgeon also had full confidence that the clinical team would not impede coronary function based on analysis using the 3D model.
Do you have a complicated patient case? Get in touch with Axial3D to request a free trial model of an upcoming or previous patient case.
Request a free anatomical visual