Aortic valve surgery made safer and faster
The Case
In this case, a 58-year-old man suffering from aortic stenosis and a recessive right coronary artery (RCA) needed an aortic valve replacement. Aortic stenosis, a narrowing of the aortic valve opening, is one of the most common and serious valve disease problems which restricts the blood flow from the left ventricle to the aorta.
Solution
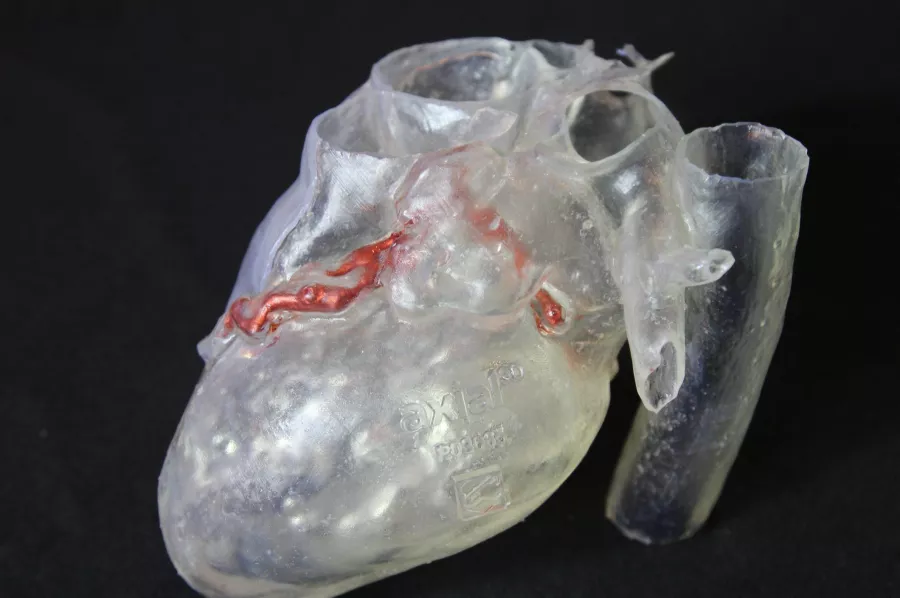
The lead physician requested a clear model of the patient’s myocardium with oversized coronary arteries to allow him to plan his procedure by injecting resin into the coronary artery to better understand how the patient’s heart was being impacted. He also hoped to allow inspection of the valve above and below and visualization of the coronary arteries using the model.

Not only did this model give the surgeon critical information and reassurance of his surgical plan, but it was also used to support a more targeted approach to selecting the equipment required for the procedure. This patient-specific model enabled the physician to see the coronary arteries in greater detail than 2D alone, which allowed him to plan the valve that he was going to implant ahead of time and ensure that it was indeed the safest route to proceed.
Benefits of using the 3D Model
By preselecting equipment the surgical team was able to save valuable time and money in the operating theatre. Crucially, this led to reduced intraoperative risk for the patient as he spent 20 minutes less on the operating table and under anesthetics than if the surgeon had not used the 3D model in planning this complex aortic valve surgery.
Up next: 3D anatomical model saves time and reduces risk on a rare transcatheter pulmonary valve replacement
Experience Axial3D for yourself
Request a free anatomical model